Bo’s Story
- You are eight years old. You have been beaten and humiliated by your stepfather for as long as you can remember. He has moved into your home, which is now a place of anxiety and fear. You feel isolated, frightened and angry.
- You are ten years old. After a night of abuse from your stepfather you seek revenge by taking some of his cocaine from the kitchen side to sell in school. You have money in your pocket and an inflated status amongst your peers. This business opportunity works well until an over-excited sixth former tells the wrong person. You become known to the police.
- You are thirteen years old. You have had six different social workers. You have stayed with different family members and also had a short spell in foster care when things got too much. Your criminal record is filling up with cautions and you have started taking the drugs you used to sell. Voices have begun sneaking into your head and encouraging you to do things that make you feel alive. Adrenaline coursing through your veins gets you through the day.
- You are sixteen years old. Education has become a distant memory. Weekdays are spent doing cash in hand work and body building, weekends are for drug and alcohol binges. You go to your mum’s house, and your stepfather verbally abuses you in front of your friends. The voices in your head are overwhelming, and a red mist descends. You take the car keys from the bowl by the front door and smash the car into a wall down the road.
- You are seventeen years old. You are arrested in possession of a firearm and a large quantity of Class A drugs. The court gives you 8 years. You complete a degree during your sentence.
Children and Young People – The Mental Health Journey
There are clearly evidenced “risk factors” that increase the likelihood of children and young people experiencing poor mental health. These include – communication difficulties, low self esteem, family disharmony, inconsistent boundaries and discipline, adults with mental health needs or substance misuse, sexual/physical/emotional abuse, parental criminality, death or loss, bullying, peer criminality, socio-economic disadvantage, homelessness, lack of access to correct support services, homelessness.
It is recorded that only 25% of children who need treatment for their mental health receive it, and that 50% of children with a lifetime condition (other than dementia) will experience symptoms by the age of 14. Young people in prison are also 18 x more likely to take their own lives than those not in a custody setting.
Conduct Disorders affect 5.8% of children between the ages of 5-16. The main factors increasing the likelihood of experiencing this disorder are being male and coming from a low income family.
Mental Health Management and Treatment within the Prison System
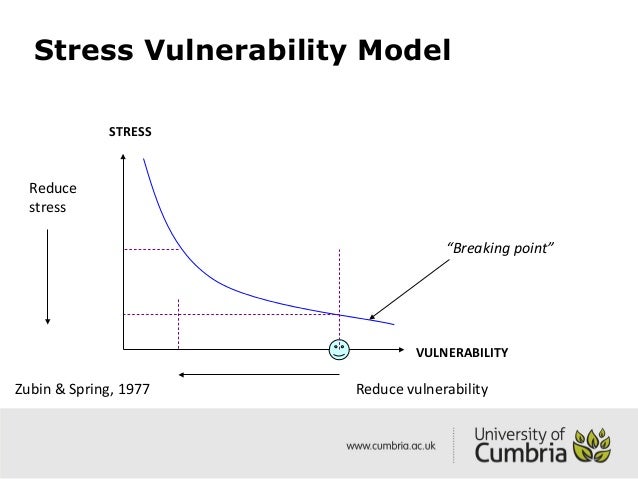
Before we explore the statistics of mental health in prison, let’s be clear. The term “mental health” refers to each and every one of us – we all have “good and/or poor” mental health in the same way we all have “good and/or poor” physical health during different times in our life. In my opinion our mental health is not a fixed state, it is a spectrum that changes based on a combination of biological, genetic, social and environmental factors. A model I tend to refer to is the “Stress Vulnerability Model” (Zubin and Spring 1977), which in simple terms is the idea is that people become mentally ill when the stress they face becomes more than they can cope with. People’s ability to deal with stress, and their vulnerability levels vary from person to person, therefore problems easily managed and resolved by one individual might be enough to cause another person to become extremely unwell.
- 70% of people who died from self-inflicted means whilst in prison had already been identified as having mental health needs. However, the Prisons and Probation Ombudsman (PPO) found that concerns about mental health problems had only been flagged on entry to the prison for just over half of these people.
- The PPO’s investigation found that nearly one in five of those diagnosed with a mental health problem received no care from a mental health professional in prison.
- The PPO also found that no mental health referral was made when it should have been in 29% of self-inflicted deaths where mental health needs had already been identified.
- 40% of prisons inspected in 2016–17 had inadequate or no training for prison officers to know when to refer a person for mental health support
The Story of “Bo”
On 9th November 2017 at 15:53 I received the following:
“I took all the tablets I had
I can’t cope with the voices anymore
I’m sorry”
During 2016 – 2017 Bo struggled to maintain long term accommodation or consistent employment, which made me wonder if there was something going on for him that he wasn’t sharing during our chats. Some days he was on top of the world, with the confidence to achieve anything he wanted; at other times he was negative, paranoid and self absorbed. I found this inconsistency very frustrating and at one point we didn’t speak for a few weeks, but we eventually fell back into our pattern of idle chit chat and world debate. I was never quite sure where he was likely to be mentally, physically or emotionally, but tried to keep an open mind and accept him for whoever, however, and wherever he was on any particular day.
9th November 2017
Bo explained to the trainee paramedic that he had been in hospital recently for a serious physical health issue, and that staff had raised concerns at the time about his mental health; but after a few extra days on the ward with no clear answers or meaningful support Bo did exactly what he always does when things aren’t going his way – a runner.
The wait in A&E was like a perverse game of musical chairs. Bo was confined to a wheelchair to reduce the risk of collapse given the vast quantity of pills he had consumed (not your typical paracetamol either, we are talking 60+ strong tablets that could do him some real irreversible damage). Every 20 minutes or so a rickety bed containing an ashen faced nonagenarian would be wheeled away, meaning we shuffled a few inches further along the crammed corridor towards wherever it was we were supposed to be going. Bo was insanely paranoid, eyeballing every passing staff member with suspicion and telling me they were planning to do something to him.
He said that he hadn’t intended on overdosing, but his original plan of jumping from a car park roof had failed when he couldn’t scale the safety fence, and the back up plan had to be aborted due to the crowds and traffic police at the railway station. Bo explained that he hadn’t wanted to ruin any more lives by allowing the train driver to hit him in front of so many passengers, but that the voices had kept telling him he needed to harm himself quickly, hence the compromise of necking all his prescribed medication.
He spent a few days on the Intensive Care Unit, (with me taking him packaged/sealed food as he was frightened the ward food was poisonous), and was then moved to the Acute Observation Ward. He refused to admit himself for mental health treatment, and so was eventually detained under Section 2 of the Mental Health Act. It was an exhausting time for us both, and my lunch breaks, evenings and weekends revolved around his visiting hours and needs. Some days he was very angry and aggressive, threatening to trash the ward if he didn’t get his own way, and on others we spoke calmly about how he was feeling. Occasionally he would be frightened, hunched in the corner of a room, unable to concentrate on what I was saying as he battled the voices in his head. Bo had no belongings with him, and so I took it upon myself to find clothing, toiletries, a phone and other bits for him to help him feel more settled (“normal?”).
The initial diagnosis was Schizophrenia, but there was talk of Bipolar and Personality Disorder too. The days turned into weeks and the weeks turned into months, and Bo’s Section 2 became a Section 3. We spent a lot of time together, and his accompanied leave eventually became unaccompanied, so we spent the time dog walking and put the world to rights like we used to.
Bo was allowed a bit of home leave over Christmas to see his Dad’s girlfriend, (which he enjoyed but found difficult due to the voices and a few hallucinations), then between New Year and January 2018 he disappeared altogether. When he finally got back in touch with me in mid January 2018, he was detained in Ashurst Psychiatric Intensive Care Unit, but couldn’t explain what had happened to result in him being there. Bo told me the professionals thought he was suffering from a Schizoaffective Disorder, with additional mood disorders similar to those associated with Bipolar. There was still no conclusive diagnosis and the medication was only partially working.
In February 2018 Bo was moved back to his original ward, and the doctors decided that maybe he had an Anti-Social Personality Disorder rather than Schizoaffective Disorder, due to his consistent lucidity prior to, and following acts of violence or self harm. As Spring approached a discharge plan into supported housing was decided – but Bo never made it to the agreed address.
In May 2018 he returned to the ward for a third time, having disappeared to a hotel on the coast to waste money on expensive food, clothes and drugs. He was told it was likely he had Psychopathy and Dangerous and Severe Personality Disorder. Shortly after his readmission to the ward Bo disappeared yet again, and his phone numbers and social media shut down entirely.
On 9th June 2018 Bo was charged with making threats to kill, possession of a bladed article, and robbery. His court date is set for 25th June 2018 (tomorrow, at time of writing), with the possibility of a long sentence ahead.
What came first, Crime or Mental Health Issues?
Perpetrators of crime must be held accountable for their actions, but cases such as Bo’s highlight continual systemic failings. He was vulnerable from a young age – a victim of abuse and adult criminal influence, a “disruptive, violent and unmanageable young man”. He received no mental health support until his first suicide attempt as an adult in his 20’s, despite clear and continuous indicators of mental health needs during his childhood. Bo has continued to “slip through the net” due to his ability to manipulate systems and say the right things at the right time, yet he is in need of intensive and enduring support. I can’t see how another long sentence will do anything to help him come to terms with the abuse he suffered as a child, the addictions of his teens and early 20’s, or the death of his mother and grandparents in recent years. A long time in prison certainly won’t help him to learn to address his difficulties in maintaining relationships, or teach him to manage a tenancy.
It needs to be recognised that suffering from complex mental health issues is not a choice. Bo is one of the most intelligent people I know, but he has absolutely no ability to control the extremes of his emotions, or make rational decisions. He is reactive, unable to plan ahead, and manages threatening or distressing situations with violence or absence. Bo has even said himself that he wonders if he has become too institutionalised to live as a functioning member of society- surviving, not thriving.
If Bo is unable to meet his “basic needs” competently (as defined by Maslow) himself due to his mental health condition (whatever the diagnosis ends up being), is prison going to help this situation? How will his sentence change his life for the better and end his cycle of offending, if his offences are linked (predominantly) to poor mental health? Being detained under the Mental Health Act has not resulted in a clear diagnosis or treatment plan that has improved his quality of life and reduced his symptoms, so do we now place the responsibility with the prison system, or do we now ignore the vulnerability he has so clearly displayed since his suicide attempt? Will a sentence exacerbate his illness, and who will be there to keep him safe?
If someone had a broken leg and an operation didn’t fully correct it, would we refuse to treat them further and then blame them for accumulating further injuries from trying to walk on it?

Prison mental health teams are faced with many challenges . Funding, staffing, and working collaboratively with the prison regime can cause complications unable to be addressed in the same way as a community setting. Research indicates that a high percentage of the prison population has a mental health need, but the behavioural challenges that arise from being unwell are often managed punitively. The PPO report published in January 2016 clearly emphasised that a lack of coordinated care between prison staff and services was a recurring theme, with sentence length and IT skills seen as particular barriers. Prisoner mental health was found to be often overlooked, due to poor information sharing, referrals not being made, inappropriate mental health assessments, and lack of staff training. Finally, a big issue explored was prisoner lack of compliance with medication, with staff not always reminding or encouraging the individual to engage with their treatment consistently.
It must be remembered that going to prison is a massive life event, and could be enough to trigger someone with previously “stable” mental health to become unwell. This change in their functioning may not be easily identifiable upon arrival in prison, and reception may assume their behaviour is “normal”. This prisoner is then left in the disadvantaged position of being unable to access personal and professional networks of support through GP appointments, phone calls and reassurance from loved ones. This leaves them vulnerable until they have the opportunity to discuss their situation with healthcare (assuming they are able to articulate the changes they are experiencing).
Study by Singleton et al 1998/2001 – Comparison of the prevalence of mental health issues across the prison population and the general population:
Schizophrenia and delusional disorder:
Prison population 8% General population 0.5%
Personality disorder:
Prison population 66% General population 5.3%
Neurotic disorder (eg: depression):
Prison population 45% General population 13.8%
Drug dependency:
Prison population 45% General population 5.2%
Alcohol dependency:
Prison population 30% General population 11.5%
What next?
How do we ensure men, women and children can access adequate support for mental health needs prior to them becoming unwell and committing crimes?
How do we improve the process for identification of mental health needs within the prison estate?
How do we encourage prison officers to work with prisoners to understand their mental health needs, and stop self harm attempts/unusual behaviours being seen as attention seeking?
How do we encourage professionals to work together and plan both sides of the prison gates (realistic and achievable outcomes), in conjunction with those with mental health needs, in order to reduce re-offending?
How do we improve professional understanding of mental health and its impact on offending and society both sides of the prison gates?
How do we make prison a place of rehabilitation and change, rather than a holding pen for the mad, bad, and dangerous?
How do we make release a time of celebration and opportunity, with meaningful opportunities and wraparound support for those with diagnosed mental health conditions?
How do we reduce the continual systemic failings and push for funding to be spent on the basics – housing, food, mental and physical health intervention, mentors, meaningful activity?
How can we encourage holistic approaches to mental wellbeing within the prison estate?
How can we find an alternative to a prison sentence for those with mental health issues who are deemed to have capacity to not be detained under the Mental Health Act?
How can we reduce self-harm and deaths in custody?
(Public Health England 2016)
(PPO 2016)
(University of Cumbria 2018)
(Prison Reform Trust 2018)
